Complete resection of tumor bearing bone with adequate margins is essential for cure.
There are two aims of surgical intervention:
- Remove the tumour with wide margins
- Reconstruct the limb to restore function
The second goal should never be placed ahead of the first – i.e. save the life, then save the limb.
A wide margin is one that has normal tissue between the plane of surgical dissection and the tumour cells on all surfaces. If microscopic disease extends to the cut surface, that is considered a microscopically positive margin.
At surgery for osteosarcoma the tumour and all contaminated tissue (including all biopsy tracts) should be excised with a wide margin
With a soft tissue sarcoma a microscopically positive margin can (in some special circumstances in experienced hands) be tolerated as there is a good local adjuvant therapy available – radiotherapy.
There is no good, effective local therapy for osteosarcomas so wide margins are mandatory to prevent local recurrence. Local recurrence of osteosarcoma is associated with a very high mortality.
Limb salvage surgery
Historically all patients received amputations, but advances over the past 40 years mean that now over 80% of patients can keep their limb and still have the tumour resected with wide margins.
The requirements of proceeding with limb salvage surgery instead of amputation are:
- Tumour margins as good as the required level amputation
- Functional outcome as good if not better than the required level amputation
- Durable result from the reconstruction (i.e. not just delaying an amputation in a couple of years)
- Acceptable to the patient
Studies of limb salvage surgery and survival are hard to interpret due to the inherent selection bias (smaller, more easily resected tumours are more likely to be in the salvage group, etc). However, survival rates seem to be similar even if some studies have suggested slightly higher local recurrence rates.
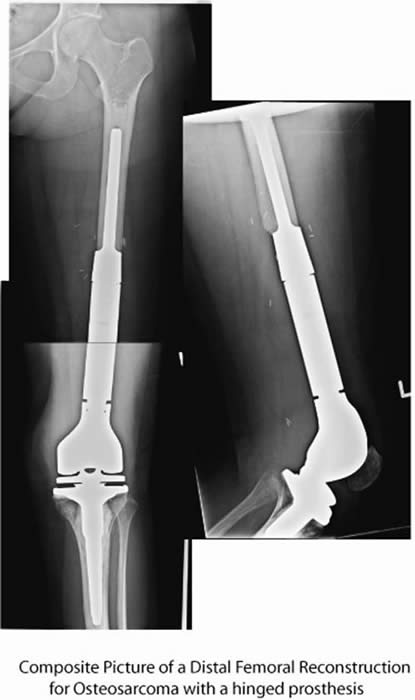
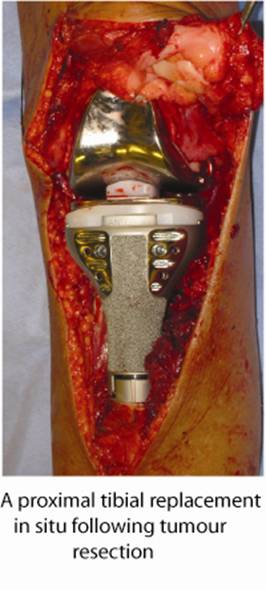
Is a combination of limb salvage and amputation. The affected leg segment is resected and then the foot brought up to the level of the knee and rotated 180 degrees and fixed into place.
The reversed foot now acts as a knee joint, and the patient wears a prosthetic leg that reaches to the ground.
The advantages are that the reconstruction does not require a joint replacement, and so does not wear out over the next 20 years. The patients function as well, if not better, than below knee amputees.
The disadvantages are cosmetic appearances and a long rehabilitation time.
This is used more commonly in children where their natural growth can accommodate changes in muscle unit length and they can adapt to their body image.
It is only rarely used for adults and it not the right option for all children; patient selection and counseling is a large part of the process.
Link: Pre-surgical video from the Mayo describing rotationplasty
Amputation
The individual patient and their parents must be heavily involved in a decision to proceed with amputation.
It is sometimes necessary if wide margins cannot be achieved or reconstruction is hampered by:
- Major neurological loss anticipated (vascular structures can usually be reconstructed).
- Major non-reconstructable bony deficit
- Major non-reconstructable soft tissue loss required.
In general the lower the tumour the lower the threshold for amputation. Below knee amputees function extremely well and will have much faster rehabilitations and return to activity than patients undergoing extensive foot and ankle reconstructions.
Patients that elect to have amputations should be referred to a specialist rehabilitation centre prior to their surgery.
Perioperatively epidural aneasthesia and co-ordinated use of long acting analgesics and nerve stabilizers not only improve the patients perioperative pain control, but may reduce long term phantom pain problems and improve their psychological acceptance of the amputation.

