Histology shows:
- Osteoid material
- Anaplastic stromal cells
Characterized by the direct formation of bone or osteoid tissue by the tumor cells.
There are 3 categories of classic OS based on the predominant differentiation of the tumor cells.
Classification of Osteogenic Sarcoma by histology:
| Classic | Osteoblastic
|
Chrondroblastic
|
|
Fibroblastic
|
|
| Telangiectatic |
|
| Small cell |
|
Classification by Location of Osteogenic Sarcoma:
| Central (Medullary) Tumors |
|
|
|
|
|
|
|
| Surface (Peripheral) Tumors | Parosteal OS:
|
Periosteal OS:
|
|
|
Conventional "classic" central osteosarcoma is the most common pathologic subtype.
Characterized by:
- Areas of necrosis
- Atypical mitoses
- Malignant osteoid tissue and/or cartilage.
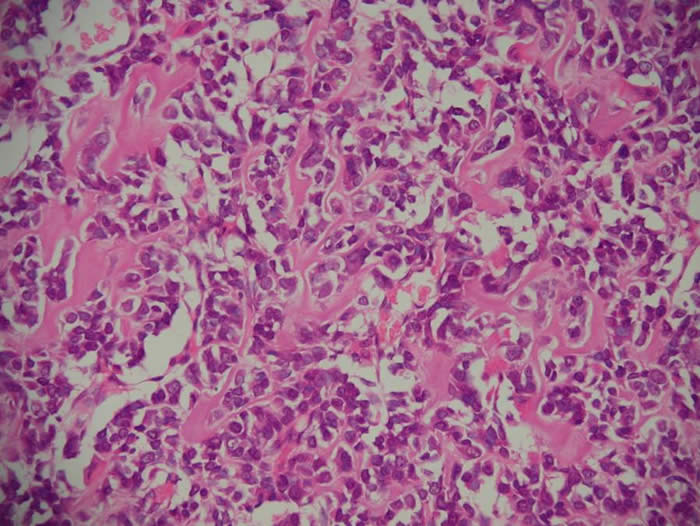
Below is a histopathology slide of osteogenic sarcoma. The pink material is osteoid. All of the malignant stromal cells are viable. This tumor is untreated.
In the past tumors were assigned a histologic grade I-IV based on the degree of nuclear anaplasia, but more recently tumors are stratified into low and high grade lesions.
To date immunoperoxidase techniques have contributed little to the diagnosis of this tumor, although some reports suggest that the identification of ‘osteocalcin’ and ‘osteonectin’ can help to distinguish osteoid from collagen [Fanburg JC et al. Osteocalcin and osteonectin immunoreactivity in the diagnosis of osteosarcoma. Am J Clin Path, 108,464-73].The other subtypes are much less common, each occurring at a frequency of less than 5%.
Recognition of intraosseous well-differentiated osteosarcoma and parosteal osteosarcoma is important:
- These are associated with the most favorable prognosis
- Can be treated successfully with radical excision of the primary tumor alone.
Related tumors include fibrosarcoma and chondrosarcoma. These also arise from primitive mesenchyme capable of differentiating into fibrous tissue, cartilage or bone.
External Link:
Osteogenic sarcoma at the Atlas of Genetics and Cytogenetics in Oncology and Haematology

