Next planning can be done either with a simulator (where plain X-rays of the treatment field can be taken) or a CT simulator (where planning CT scan images can be generated and treatment can be planned in 3 dimensions).
CT Simulator:
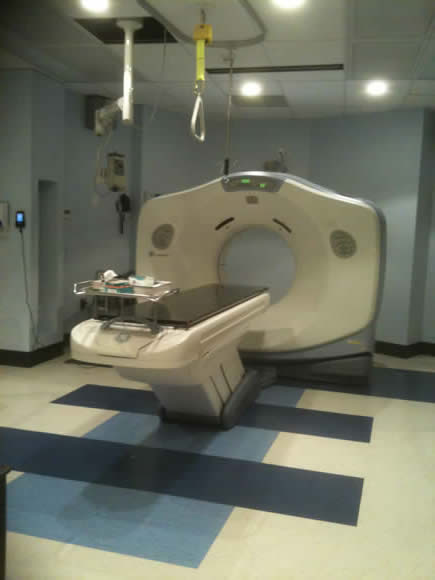
This is a dedicated CT scanner for planning radiotherapy (RT) and is used to plan radical RT in three dimensions.
Multiple cross sections are generated and it is possible to identify structures and draw on the CT images at multiple levels.
The structures targeted include:
- The tumor
- Critical normal structures adjacent to the tumor:
- Normal tissues can only tolerate a certain amount of radiation before serious damage is sustained
- Some normal tissues are very sensitive to RT (such as the kidney) and others are more resistant to the effects of RT (such as peripheral nerves)
Then the radiation oncologist as part of a team with Medical Physicists and Radiation Therapists designs a treatment plan.
- Plan designed to treat the tumor to a high dose and avoid critical normal structures.
- The radiotherapy fields enter or “come in” from different angles around the patient to treat the tumor and spare surrounding normal tissues.
- CT planning enables one to see how the treatment plan looks inside the patient.
Image Fusion Techniques
Some radiation therapy departments use MR simulation on a routine basis for patient planning. For those centers that do not possess a MR simulator, image fusion techniques can be used to plan RT.
Image fusion techniques can be used to identify tumor location.
- Many tumors are better seen on MR - especially soft tissue sarcomas.
- Sometimes RT needs treat the initial extent of the tumor before chemotherapy. After treatment, when the tumor has shrunk significantly, it can be very hard to identify the extent of the tumor at first.
MR scans can be fused with the planning CT scan images to give the most precise picture of the extent of the tumor. CT/MR fusion techniques are easy to use in the head and neck because bony landmarks (base of skull) can be used to merge the two image data sets perfectly.
It is possible to use CT/MR fusion in other areas of the body - but the MR should be done in the same position as the CT planning scan or the overlay (matching) may not be as accurate.
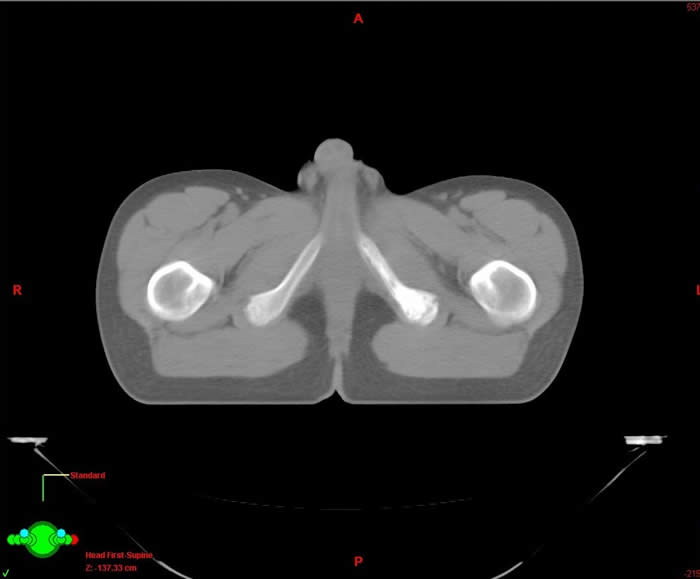
Below is a CT planning scan for RT. The scan was done after chemotherapy for treatment of large pelvic Ewings sarcoma. It is very difficult to see any abnormality or to know where to direct the radiotherapy.
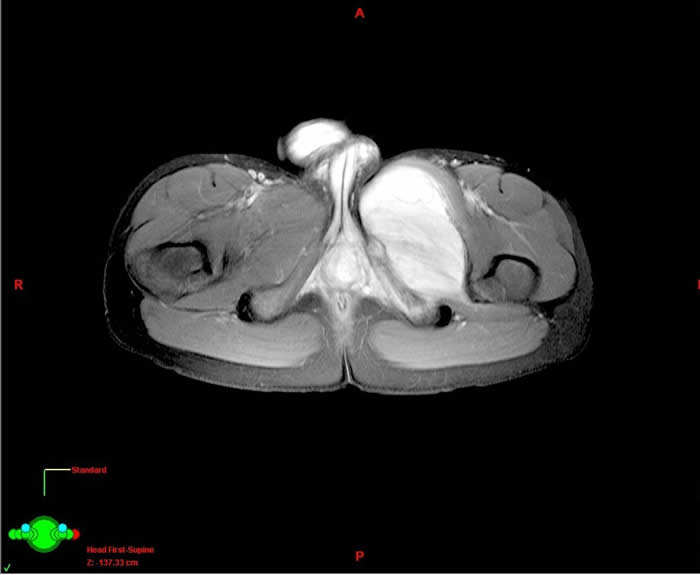
Here is a MR image which clearly shows the original extent of the Ewings sarcoma. This can be overlaid on to the CT planning image above and used for treatment planning.
Other methods to locate the tumor bed :-
- It is very important for the radiation oncologist to be involved with the treatment plan almost as soon as the patient's tumor has been diagnosed. Examination of the tumor at presentation gives a really good idea of the extent of tumor prior to any chemotherapy.
- Good communication with the Radiologist - review films in person with radiologist.
- Good communication with the surgeon:
- Talking directly about the findings at surgery.
- If the surgeon places clips at the time of resection - these can later be seen on the CT planning scan and help to identify the tumor bed.

