Typhlitis
Also called Neutropenic Enterocolitis”or “Necrotising Colitis”
Inflammation of the cecum that can lead to infarction and perforation.
The cecum is the most common location for this to occur, but it can occur in any part of the large intestines.
- Intraluminal bacterial invasion of bowel wall mucosa
- Inflammation → infarction → perforation
- Only in profoundly neutropenic patients
- Cecum usually involved
- Usual Bacteria: Clostridium Septicum or Pseudomonas Aeruginosa
Signs
- Fever and right lower quadrant pain and tenderness
- Partial obstruction
- Right lower quadrant mass
- If there is a perforation, the patient often becomes very unstable and develops a rigid tender abdomen.
Patients who are on high dose steroids (such as those on treatment for ALL) may have masking of the signs of tenderness and rigidity of the abdomen.
Investigation
- Blood work - CBC ( profound neutropenia), lytes, BUN and creatinine. Blood cultures.
- Abdominal X-ray shows air in thickened bowel wall, “railway track appearance” or pneumatosis intestinalis
Management
- Broad spectrum antibiotics
- No oral intake (nasogastric tube and suctioning)
- IV Fluids, electrolytes and blood products as needed.
- TPN if necessary
- Pain control
- For the child who has a perforation, urgent surgical assessment is required.
- Surgery is only as a desperate last resort if there is:
- Continued and severe GI bleeding
- Evidence of perforation and free air in the abdomen
- Uncontrolled sepsis from bowel infarction
Sometimes the signs of typhlitis are not very impressive or masked by steroids.
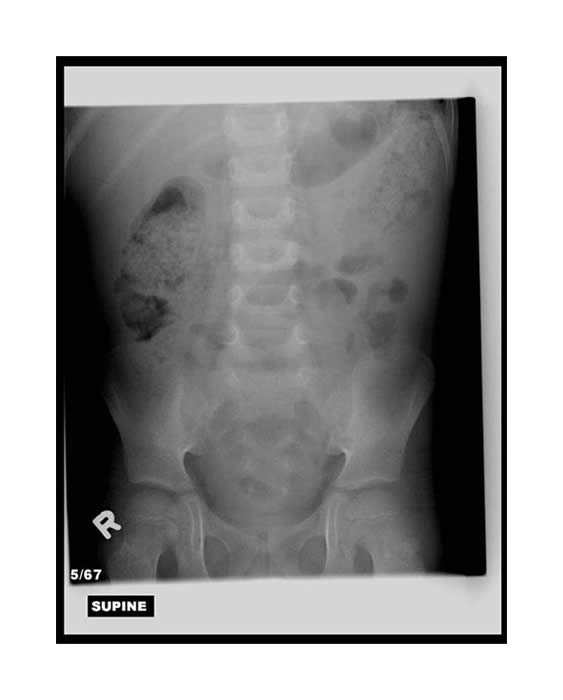
The plain film below was taken on a child who was seen in clinic for abdominal pain on day 23 of induction therapy of Acute Lymphoblastic Leukemia (ALL).
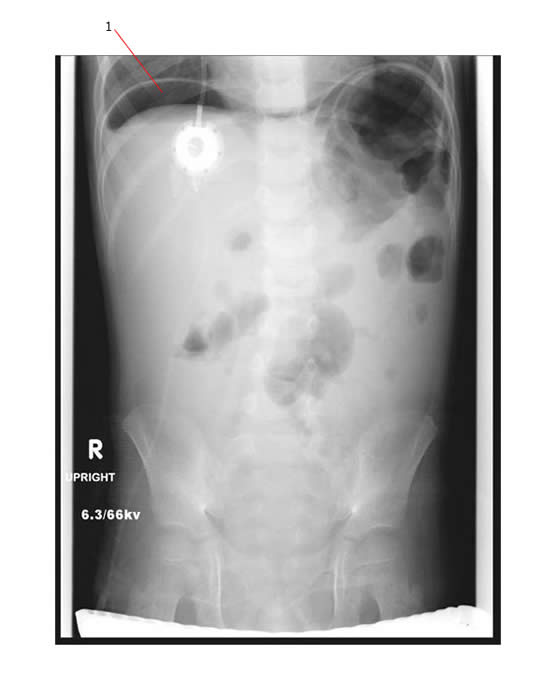
Below is a plain film of the same patient taken 2 days later when he was seen in ER with worsening abdominal pain (but no peritoneal signs !!!) . Note the gas under the diaphragm (#1) which indicates a bowel perforation.